Practising Evidence-Based Dentistry (EBD)
The five-step approach to teaching EBD is a structured (stepwise) process for dealing with clinical problems
The Evidence-based approach is essentially a structured (stepwise) process for dealing with clinical problems. This stepwise approach encourages the use of the latest information rather that a reliance on techniques, materials and treatments learned years earlier.
There are five elements to the approach. Select each tab below to find out more:
- Question: Developing a clear question based on the patients clinical problem.
- Find: Finding the latest evidence through efficient searching for information.
- Appraise: Critically appraising the evidence to assess its value.
- Act: Acting on the evidence you find, if appropriate and relevant to the clinical situation to provide treatment for the patients.
- Evaluate: Each aspect of your performance in this process can (and should) be evaluated and this is increasingly relevant with the development of continuing professional development.
A closer look at each of the five steps:
Question
In practice it is a rare day when you are not faced with a need to know some new information about the prognosis, treatment or management of a condition. Turning these clinical problems into a well-built (answerable) clinical question is a key skill of evidence-based practice.
There are essentially two types of question:
Background questions
These ask for general knowledge about a disorder and have two main components.
- A question root (who, what, how, when or why)
- A disorder or specific aspect of a disorder (e.g. What causes dental caries? or What are the complications of root canal treatment?)
Foreground questions
These ask for specific knowledge about how to manage patients with a disorder and a good or well-constructed foreground question usually has four main elements:
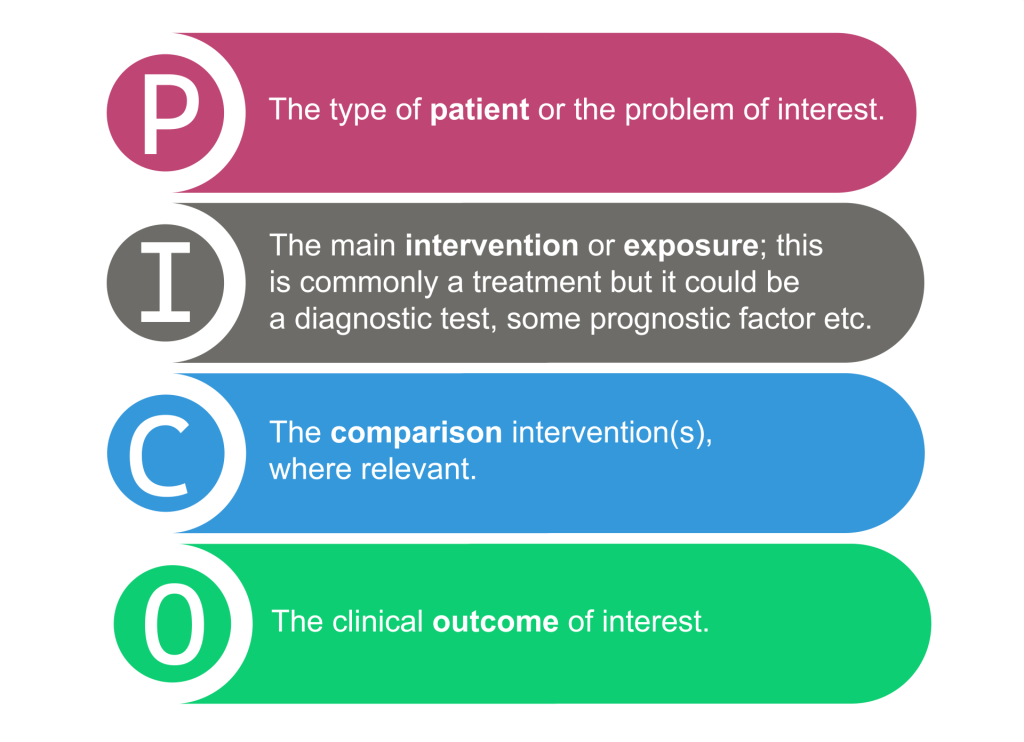
Commonly referred to as PICO or PECO format (e.g. in patients with tooth discolouration would home bleaching compared to placebo lead to whiter teeth?)
Resources
- Focusing Clinical Questions – from Centre for Evidence-based Medicine UK.
- Developing answerable clinical questions -Terry Shaneyfelt ( YouTube)
Find
How to find evidence
We are constantly bombarded with information from a wide range of sources. Traditional sources of information (books, journals and colleagues) as with other sources have their limitations.
With the rise of the internet, an increasing number of electronic databases are available which can provide access to the best current evidence. The most widely available free database is Medline which can be accessed via the PubMed interface. Increasingly databases are providing explicit evidence; a good example is the Evidence-based Medicine reviews product from Ovid, which combines a number of electronic databases (Cochrane Database of Systematic Reviews, Best Evidence, Evidence-based Mental Health and Evidence-based Nursing, Cancerlit, Healthstar, Aidsline, Bioethicsline and Medline).
The Cochrane Library is a collection of databases that contain different types of high-quality, independent evidence to inform healthcare decision-making.
- The Cochrane Database of Systematic Reviews
- The Cochrane Central Register of Controlled Trials (CENTRAL)
- Cochrane Clinical Answers
The Cochrane Library is probably the best single source of reliable evidence about the effects of healthcare.
Structured approach to searching
In order to be really effective in searching for evidence, specific training or access to an information specialist is required. However, for a busy practitioner a quick structured approach is:
First define the question – then search for each of the following in turn:
- Evidence-based Guidelines
- Cochrane Reviews
- Evidence summaries (e.g from Evidence-based dentistry Journals, The Dental Elf)
- Medline – for appropriate studies to answer your question.
Relevant Links
- Levels of Evidence: An Introduction from the Oxford Centre for Evidence-based Medicine
Resources
Papers on searching from the Canadian Dental Journal series on Evidence-based Dentistry
- Part II. Searching for Answers to Clinical Questions: How to Use MEDLINE – Susan E. Sutherland
- Part III. Searching for Answers to Clinical Questions: Finding E-vidence on the Internet – Susan E. Sutherland & Stephanie Walker
- PubMed FAQ– Frequently asked questions about PubMed from NCBI
Search filters
Databases
- Centre for Reviews and Dissemination-(University of York) – databases
- Clinical Trials Register USA
- Cochrane Library
- CORDIS Community Research & Development Information Service – European Research
- Medline (PubMed)
- MetaRegister of Controlled Trials searchable, international database of ongoing trials ( ISRCTN Registry)
Search Engines
- Epistemonikos – a collaborative, multilingual database of health evidence. It is the largest source of systematic reviews relevant for health-decision making, and a large source of other types of scientific evidence.
- TRIP Turning Research into Practice – Excellent UK based meta-search engine
Other
- Ovid Medline Tutorial for Dentistry – from Faculty of Dentistry, University of Toronto
Appraise
Appraising the evidence
Almost all scientific studies are flawed and it would come as a surprise to some clinicians that some (perhaps most) published papers (ref 1) should be thrown in the bin rather than used to inform clinical practice.
Critical appraisal is a way of rapidly assessing published papers in order to sort out the relevant or valid papers from the poor quality or irrelevant ones.
Validity – is the degree to which the results of the study are likely to be true, believable and free from bias.
Bias – is any factor (other than the experimental factor) that could change the study results in a non-random way.
Critical appraisal is best carried out in a structured/standardised way using explicit criteria. Appraisal can help the clinician to assess:
- Validity
- Clinical importance
- Clinical relevance
References
Resources
- AMSTAR -Assessing the methodological quality of systematic reviews
- Appraisal of Guidelines Research and Evaluation AGREE
- CASP (Critical Appraisal Skills Programme) and Appraisal tools
- Critical Appraisal Skills Programme Español
- Critical Appraisal tools list – from iCAHE – Australia
- CAT Maker software tool for Critically Appraised Topics – Oxford Centre for Evidence-based Medicine
- CEBM Oxford- Critical Appraisal tools page – appraisal sheets and calculators
- Dental CATs (Critically Appraised Topics) from University of Texas Health Science Center
- DISCERN. – Instrument for assessing a consumer health information
- EQUATOR Network – resource centre for good reporting of Health research studies
- SIGN Algorithm for classifying study designs
- SIGN Critical Appraisal checklists
How to Read a Paper series (1997) by Trish Greenhalgh from The British Medical Journal
( In order to access these BMJ articles you will need to register with the BMJ )
- The Medline database
- Getting your bearings (deciding what the paper is about)
- Papers that report drug trials
- Papers that report on diagnostic or screening tests
- Papers that summarize other papers (systematic overviews and meta-analyses)
Papers on appraisal from the Canadian Dental Journal series 2001
- Evidence-based Dentistry: Part V. Critical Appraisal of the Dental Literature: Papers about Therapy – Susan E.Sutherland
- Evidence-based Dentistry: Part VI. Critical Appraisal of the Dental Literature: Papers about Diagnosis, Etiology and Prognosis – Susan E.Sutherland
Study Design Series by Kate Ann Levin in the Evidence Based Dentistry Journal
- Study design I. Evid Based Dent. 2005;6(3):78-9.
- Study design II. Issues of chance, bias, confounding and contamination. Evid Based Dent. 2005;6(4):102-3.
- Study design III: Cross-sectional studies. Evid Based Dent. 2006;7(1):24-5
- Study design IV. Cohort studies. Evid Based Dent. 2006;7(2):51-2.
- Study design V. Case-control studies. Evid Based Dent.2006;7(3):83-4.
- Study design VI – Ecological studies. Evid Based Dent.2006;7(4):108.
- Study design VII. Randomised controlled trials. Evid Based Dent.2007;8(1):22-3.
Other
- Teaching critical appraisal skills in health care settings (Cochrane Review Abstract),
- Statistics at Square One (BMJ Publications)
- Hazard ratio tutorial – from Students4best evidence
- Surrogate Endpoints – from Students4best evidence
- EQUATOR Network – Transparent reporting of health research – You tube video of webinar
- Terry Shaynefelt critical appraisal videos
Act
Acting on the evidence
Being aware of the available evidence is one thing, but acting on it is another.
There are a number of well documented delays between clinical practice and the available research evidence. The most often cited examples have been in medicine but one can look at the variations in the use of topical fluorides and fissure sealants despite good evidence of their effectiveness. These delays and variations in provision and uptake of treatments have contributed to the development of the evidence-based approach.
The practitioner needs to decide whether the specific patient is similar enough to those in the research to use the findings. There may also be barriers regarding the materials or equipment required, and there may also be cost implications. There are also personal barriers such as the extent to which the results conflict with professional experience and cherished beliefs (see list of resources below).
The decision to act on evidence should be based on the evidence, the relevance to your patient, the willingness of the patient to receive the treatment, and the practitioners ability to provide the treatment. It is therefore a carefully considered decision and not a ‘cookbook’ approach, as has been claimed by some opponents of evidence-based practice.
Resources for acting
Getting Research Findings into Practice Series from: The British Medical Journal (Now also available as a book)
- Making Better use of Research Findings
- When to Act on Evidence
- Finding Information on Clinical Effectiveness
- Barriers and Bridges to Evidence-based clinical practice
- Using research findings in clinical practice
- Decision Analysis and the implementation of research findings
- Closing the gap between research and practice
- Implementing research findings in developing countries
Evaluate
Evaluating your performance
The final step of the evidence-based approach is self-evaluation. In their Evidence-based Medicine textbook [1]. Sackett et al. suggest a number of self-evaluation questions for each stage of the evidence-based approach. A few examples are shown below:
- Question
- Am I asking any clinical questions?
- Are they well structured?
- Finding
- Am I searching for evidence?
- Do I know what the best sources are?
- Am I getting better at it?
- Am I finding evidence?
- Appraisal
- Am I critically appraising evidence?
- Am I getting better at it?
- Act
- Am I using evidence I find and appraising it in my practice?
References
- Sharon Straus Paul Glasziou W. Scott Richardson R. Brian Haynes. Evidence-Based Medicine: How to Practice and Teach EBM. 5th Edition. Elsevier 2018.